Orthoptists are experts in diagnosing and treating defects in eye movement. They meet patients with a broad range of eye conditions that affect vision, offering treatments to help the eyes better function.
The VisAbility team includes Orthoptist Amy Crosby. As a child, Amy’s sister was born with a squint – a condition known as strabismus. Amy remembers her sister attending appointments for glasses, the surgeries she had to straighten the eyes, and patching treatment to avoid amblyopia (lazy eye). It’s just one of many reasons she has followed a career in orthoptics.

“People see me after they have had a diagnosis with an ophthalmologist. It’s my job to see how the eyes are working. I assess their vision function and can recommend solutions to improve their vision such as magnifiers. I can also offer other strategies such as isolating text if lines appear to run over each other.”
Amy trained at the University of Sydney (link opens in new window) and completed a Bachelor of Applied Science (B.App.Sc) in Orthoptics, graduating in 2006. Before working at VisAbility she worked at a general ophthalmologist practice. She is married and has two young children – a seven-year-old son and a five-year-old daughter.
“I love this role because I see both adults and children who live with vision impairment. Children can be more complex because they can’t express themselves so easily. With adults, you’ll see people who’ve lost their sight, maybe through old age, and are going through a grieving process, so that can be equally as challenging.”
To mark this month’s World Orthoptic Day, Amy shared a snapshot of her working day.
0900-1030 – Presentation to therapists
I give a presentation at a monthly meeting with the therapists from our Children and Youth Services about children’s vision and how I assess a child’s vision.
The therapists are from all areas of our organisation and include occupational therapists, speech pathologists, dietitians, and physiotherapists. My presentation offers valuable insights into the different examinations I might conduct, and how various diseases affect the eyes. I explain some of the terminologies I use in my job – such as visual acuity, visual field, depth perception and ocular motility.

The floor is opened up to questions. I get asked about a newborn’s vision and expected milestones up to a year. Many people aren’t aware that babies have limited vision when they are first born.
Another person asks whether I can examine someone’s eyes and produce a classification so they can swim in competitive multi-class (disability) swimming competitions. There are three different sport classes for athletes with vision impairment, numbered S11-13. A lower number indicates a more severe limitation. I hope to be authorised to do this by the end of this year. I need to be trained by the Paralympics Classification Service, and they’ll be offering more courses after the Tokyo Olympics.
11:00 – 12:00 – Client – Charlee
My first client is six-year-old Charlee. She has a range of disabilities and uses a wheelchair, and requires a vision assessment. Now Charlee is in year one at school, I’m looking at options to help her in the classroom. She has support from an educational assistant. Charlee has poor vision in her left eye, and her mother explains that she holds things close to see them.
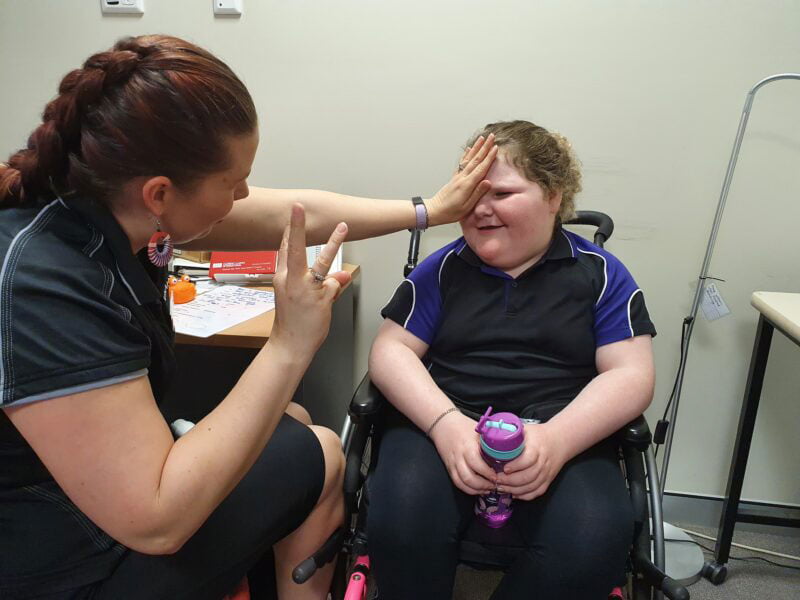
I undertake an eye examination and carry out several tests using shapes that diminish in size. I also check for colour blindness and contrast. Lighting and magnifiers can be so beneficial to young people, and I demonstrate a few.
I will prepare a report to send to her ophthalmologist.
13:00 – 1430 – Client – Glen
Glen is a new client, 59-years-old and has Down’s syndrome. My notes tell me Glen is non-verbal, which can be challenging.
When I meet Glen and his support worker, who’s been with him for nine years, I discover he can communicate a little. Between the three of us, we find out about his sight.

Glen has esotropia – a form of strabismus – in which one or both eyes turns inwards. He has glaucoma and uses daily drops for his dry eyes.
The vision on his right side is not very good. He has reduced vision field loss that has impacted his day-to-day life, and bumps into obstacles such as furniture and door frames in unfamiliar areas. Glen also spills his food when he eats.
Glen had some laser surgery more than a decade ago and now has three-monthly eye appointments at the Perth Royal Hospital.
I undertake numerous tests, including visual acuity and eye movement.
15:00 – 16:00 – Client – Anna
My final client of the day is three-year-old Anna with ocular albinism.
Ocular albinism does not affect skin colour and hair but does affect the sharpness of vision. Anna has an involuntary movement of eyes back and forth – known as nystagmus.
Her mother explains that she brings things close to her eyes to look at them. I examine Anna’s eyes, undertake a variety of tests for visual acuity and colour blindness as well as a stereo-fly test. I offer Anna some of my ‘magic glasses’ to wear to do this test. Their purpose is to measure how the two eyes can manage differences in distances.

Anna’s close vision is good. It’s her long vision that is worse. She’s about to go into kindy, so we talk about the assistance she can get at school and how we can make life easier for her in the classroom, support available, and other early intervention services that may help.
I tidy away after the appointment and make some notes. No two days are ever the same.
I know that I’m making a difference with my role. From explaining eye conditions so clients have a better understanding of how their eyes function, to investigating magnifiers or strategies to enhance their vision – it’s a varied role.
I can also suggest other specialists or counselling options. If I had my time again I’d still do this job, which is both hugely satisfying and rewarding.
Our orthoptists receive accreditation from the Orthoptic Board of Australia (link opens in new window). Find out about what we offer and get in touch today.
How to get support
We can help you to make the most of your remaining vision. Please complete the form below to make an initial enquiry about the low vision services and support we can provide. Our Client Experience Team will contact you to discuss your individual needs both now and into the future.
If you are a provider and wish to refer a client, please use our low vision medical certificate (online referral form) to make your referral.
.
